|
|
|
|
Creatine
Basics and Biochemistry
Many
weight training enthusiasts would likely agree that amongst nutritional
supplements, creatine monohydrate is perhaps one of the most popular on the
market today. Nutritional stores, athletic shops, and even grocery stores
have begun to carry creatine. Numerous manufacturers produce the product,
which can be delivered in a variety of methods, including liquid, powder, and
capsule forms. How did
the obsession with creatine begin? In 1992,
at the Olympic Games in Barcelona, some athletes competing in sprinting and
power lifting events made some claims that creatine supplementation helped
their performance. Subsequent to these claims, many studies were conducted
regarding supplementation with creatine, and its popularity grew
substantially in the United States. Understanding
the function of creatine requires a basic knowledge of biochemistry.
Specifically, one should refer to our article entitled "Basic
Metabolism" for further information. Basic metabolism is outside of the
scope of this paper. Creatine
basics: Creatine,
or methyl guanidine-acetic acid, is an endogenously formed (made within the
organism during natural metabolic processes) molecule that is stored largely
in skeletal muscle, in both free and phosphorylated forms. The phosphorylated
form of creatine is appropriately termed phosphocreatine or creatine
phosphate. Because of its abundance in these tissues, it is not
surprising that people who consume non-vegetarian foods subsequently consume
larger quantities of creatine, which can be digested and stored in their own
muscles. In skeletal muscle, the concentration of creatine is approximately
125 mmol/kg dm. Of note, creatine is also found in the brain, liver, kidney,
and testes in much smaller quantities. During
high intensity exercise, the muscle ratio of ATP:ADP (adenosine
tri-phosphate:adenosine di-phosphate) decreases drastically, due to
consumption of high-energy phosphate groups from ATP. Muscle failure is
associated with the decrease in ATP:ADP ratio during short bouts of
high-intensity anaerobic exercise, such as in resistance training. Creatine
plays a key role in maintaining a high ATP:ADP ratio by phosphorylation of
ADP1, thereby delaying muscle fatigue and allowing for prolonged
high-intensity exercise: Creatine
phosphate + ADP + H+↔ creatine
+ ATP Muscle
concentrations of creatine phosphate are typically quite higher than
concentrations of ATP. Therefore, the above equation would tend to consume
the reactants (creatine phosphate) to produce more product (ATP) in order to
balance the system. Studies have clearly documented the benefits of dietary
creatine supplementation, which is theorized to cause a substantial increase
of phosphocreatine levels in type II (fast-twitch) skeletal muscle fibers. In
fact, studies approximately 80 years ago confirmed the retention of creatine
by the human body via dietary supplementation2. Creatine
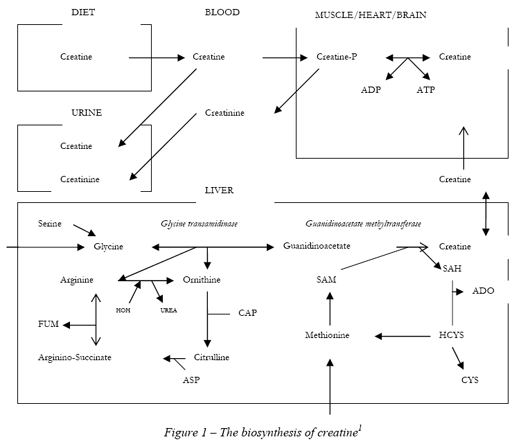
biochemistry: The
majority of in vivo creatine synthesis takes place in the liver. The first
step involves transfer of an amidine group from arginine to glycine by the
enzyme glycine transaminidase. The resulting guanidinoacetic acid is
methylated via guanidinoacetate methyltransferase (with the methyl group
coming from S-adenosylmethionine) to form creatine. The creatine is then
transported via the bloodstream to storage sites in skeletal muscle (95%),
where it can be phosphorylated via ATP to form creatine phosphate. Dietary
creatine is transported from the gastrointestinal tract to the appropriate
storage tissues as well. About 60%-70% of the creatine in skeletal muscle is
phosphorylated, thereby preventing migration across the plasma membrane, and
essentially trapping the molecule within the muscle cell.
The
degradation of creatine is of particular clinical interest. The only end
product of creatine degradation is creatinine, which diffuses into the
bloodstream from the muscle. Upon entry into the renal parenchyma, creatinine
is filtered in the glomerulus and excreted in the urine. Therefore, the
clinician must be weary when interpreting the basic metabolic panel from an
individual with large amounts of muscle mass, or in patients supplementing
their diets with creatine. Such patients will exhibit elevated creatinine
levels in the blood, and therefore, their blood creatinine levels may not be
accurate indicators of renal function. The
methods of dietary creatinine delivery (i.e. powder vs. solution vs. tablets,
loading, etc. are outside the scope of this article. Risks
of Creatine Supplementation: As noted
earlier, elevations of plasma creatinine found in patients who supplement
their diets with creatine are not indicative of renal function. Therefore, it
is not appropriate to rely on creatinine levels in such patients for
diagnosis of renal failure. On a positive note, some studies have failed to
report changes in serum markers of hepatorenal function following chronic
creatinine supplementation3,4. More information regarding the risks of
creatine supplementation will follow in subsequent publications. References: 1.
Greenhaff, PL. (1997). The nutritional biochemistry of creatine. Nutritional
Biochemistry 8:610-618. 2.
Chanutin. A. (1926). The fate of creatine when administered to man. J. Biol.
Chem. 67, 29-37 3.
Earnest. C., Almada, A.. and Mitchell. T. (1996). Influence of chronic
creatine supplementation on hepatorenal function. F.A.S.E.B. 10,4588 4. Almada,
A.. Mitchell, T., and Earnest. C. (1996). Impact of chronic creatine
supplementation on serum enzyme concentrations. F.A.S.E.B.10,4567 |
|
|||||||||||||||||||||||||||
|
© Copyright 2005-2009 University
of Michigan Board of Regents and MedFitness Group |